Shifting the stigma
Changing discussion around mental health and mental illness
“Stigma is a sociological concept ... (sociologist) Erving Goffman says stigma actually is a powerfully negative social label that radically changes the person’s self-concept and how they understand themselves and their social identity.” – Christopher J. Fries
Stigma surrounding taking medication for mental health and mental illnesses, as well as stigma around mental health in general, has decreased in recent years. This shows through both sociological and medical points of view.
“I think the attitude towards mental health has really changed in the last couple of decades,” Carl Heaman-Warne, director of therapy at Aurora Family Therapy Centre, says. “And certainly, we see much equal numbers in men and women looking for help now. I think that wasn’t true in the same way 20 years ago.”
Christopher J. Fries, a professor of sociology at the University of Manitoba who studies population health, also agrees more people, including his students, are open to talking about mental health. However, from a sociological perspective, he can also see some problems with society being so open.
Fries is an assistant professor of sociology at the University of Winnipeg.
From a population health level, Fries says that “when everyone starts to interpret what’s happening in their lives in terms of their neuro-chemistry instead of asking themselves, ‘maybe it’s the structure of my society that’s making me sad’
… That’s sociological, that’s what’s dangerous about medicalization.”
Medicalization is a part of the process of stigma around mental health decreasing. Fries describes it as defining troubling aspects of life from behaviour to unpleasant emotional states as medical issues that require medical attention.
“There’s no doubt that mental illness exists objectively,” Fries says. He adds that the suffering people experience through mental illness is very real. “I would also go as far to say that I know from my own experience with friends and even family members (who) are indeed saved, like their lives are literally saved by these psychotropic (pharmaceutical) drugs.”
Being able to openly have conversations about mental health can encourage those who need help to get it.
“Just the fact that we’re willing to talk about it now, so openly, shows that it has become destigmatized,” Fries says. “And I’m not saying that’s all bad. Again, for people who have profound mental illness, that’s a good thing. People are now able to seek out help and treatment for it.”
Pushing stigma aside
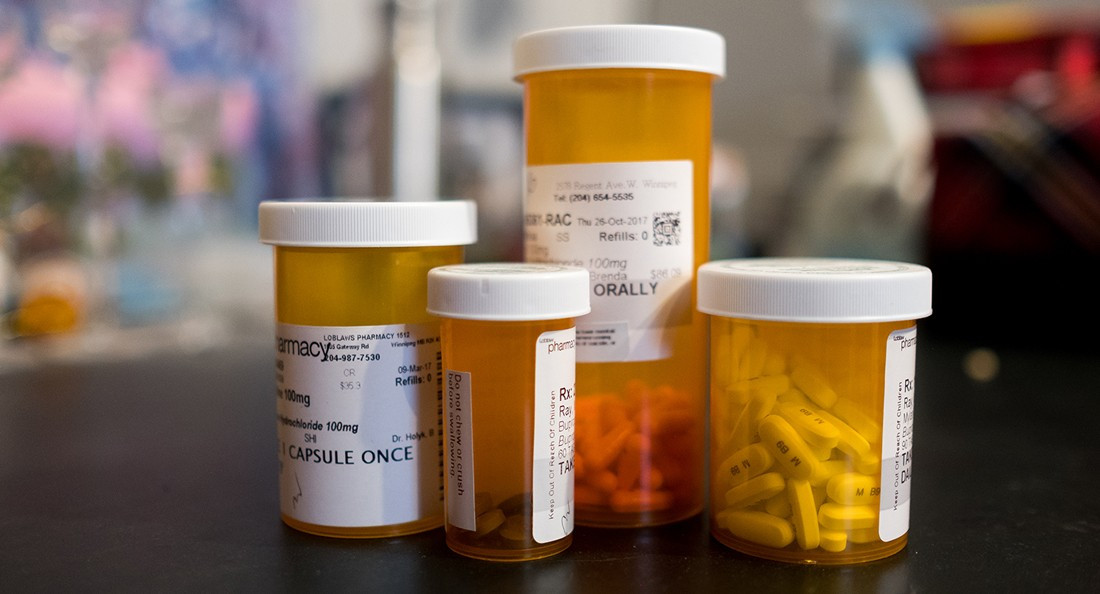
Melissa Ray says they have social anxiety and have been using both pharmaceutical medication and medical marijuana for their mental illness.
“I was happy to have something to make me feel better, but it also made me feel like all the things that I thought were wrong with me were actually wrong with me,” they say. “I wasn’t going crazy. I was really happy to go on medication, because it was really validating.”
Ray says before they started taking medication, they had a lot of unhealthy coping mechanisms like self-harming, eating junk food and self-sabotaging.
Melissa Ray has been taking medication for mental illness for several years.
When it came to stigma around mental illness and medication, Ray was ready to push that aside.
“I was really determined to be open about it. I really don’t like the idea of being shameful about my mental illness,” they say. “I think (stigma is) a really old-fashioned idea, and I think it’s a stigma that’s thankfully on its way out. I think a majority of younger people understand that that’s just ridiculous.”
Taylor Janzen, who is 18 and a local musician, also pushed the notion of stigma aside when she started taking medication for her ADD.
“Taking medication was like putting on glasses for my brain,” she says.
“I don’t think I was ever necessarily ashamed of it, because I have a very small ability to be embarrassed about things,” she says. “I’m a very special person. I don’t get embarrassed about anything. I talk about everything all the time, which is why my music is so intense.”
Janzen was diagnosed with ADD when she was in Grade 12. She says she had been diagnosed three or four times before this final diagnosis, but the diagnosis was always taken away and changed.
She was bounced between about seven psychiatrists and family counsellors when she was 16.
“They had to hear all of my darkest thoughts and my worst experiences,” she says. “It was very exhausting to keep bringing that up to new people and exhausting to keep thinking that you had something and have that taken away.”
Her song “The Waiting Room” talks openly about her experiences seeing therapists and taking medication – more specifically, about the flaw in the medical system that contributed to her being bounced around so much.
“At first I thought it was just me. Like am I some weird jigsaw puzzle that no one can figure out? But then I realized, no, I’m a human being, and it must be a flaw in the system, because I can’t be the only person actually experiencing this,” Janzen says.
Stigma and health
Heaman-Warne says part of stigma is an acceptance process of facing the challenges people come across in their lives.
“If we think about any kind of grief process, the first part of those grief processes is ‘no, that’s not me, if only I did x, y and z instead, then this wouldn’t actually be real. I won’t actually have to deal with depression, or I won’t have to face anxiety, or it won’t actually be trauma. Maybe I need to go to yoga more, or maybe I need to have more greens in my diet. Maybe I just need to talk to a friend,’” he says.
Lifestyle shifts aren’t always enough, and part of the acceptance process is knowing you need help.
“We need some help from outside of ourselves. And whether that help is counselling or it’s medication or some kind of plan, almost everybody pushes away from that initially,” he adds.
Heaman-Warne says people sharing their own stories and struggles helps to normalize mental health challenges.
Fries says his sociological concern with more people being open about talking about mental health, mental illness and medication is that more people are now being marketed for psychotropic medications. People become the item on the market for pharmaceutical companies.
Rather than changing problems in society to help mental health issues, pharmaceutical companies are using the increase in mental health issues for their own profit.
Instead of looking at a societal level of problems, people are turning towards medication.
“It turns troubling aspects of life into medical issues and keeps us from understanding that it could be more than medical issues,” Fries says.
Stigma at home and in communities

Some of Melissa Ray's medical marijuana.
Although Ray is open publicly and on social media about their mental illness, they says they still deal with stigma in their own household, especially with their use of medicinal marijuana.
“I guess the main issues I’ve had with stigmas and smoking marijuana was in my own household, because I still live with my parents,” they say. “It’s a really old-fashioned stigma that people have embedded in them that marijuana is bad, and that’s it.”
They say their dad wanted them to get their medical marijuana card so they could get their marijuana medically prescribed to them. But even with that, they say he was still in their face and shameful about it.
Ray says there’s a difference between generations when it comes to talking about mental health and medicinal marijuana.
“Older generations just want to be shamed about everything. And it’s like ‘no thank you,’ I don’t like the heavy depressingness of shame,” Ray says.
Janzen has also noticed some stigma and people being uncomfortable with talking about mental health in her communities, but it’s not based on age demographics.
“I grew up in a really religious community, and religious people specifically … get uncomfortable when you talk about mental health,” she says.
She adds that when she was younger, she struggled with her faith and her mental health issues.
“When I was growing up, when I first experienced mental health issues, it was very difficult, because I was trying to fight it off in a way, because I had an impression that it was like, if you had a proper relationship with God, if you were a proper Christian, then you didn’t have mental health issues,” Janzen says.
Janzen realized having mental health issues wasn’t her fault, and this ultimately made her faith stronger.
“And that’s not true. So I basically assumed it was my fault. When I started taking medication, I felt really uncomfortable, because was my faith not enough to make it alright?” she says. “But now I’ve found a cool way to integrate those, and taking medication has actually made my faith stronger and made my personal goals more reachable and attainable. So that’s really cool.”
Culture shift in stigma
Through a sociological lens, culture and society have played roles in how the conversation around mental health in general has shifted.
“Why I feel sociologically confident in saying there’s social and cultural basis to these mental illnesses is because we know that across time, and also more importantly across culture, the rates of these mental illness or mental disorders changes,” Fries says.
Janzen also believes that how people relate to their mental illness, and how she sees hers, is dependant on society’s view of mental health and mental illnesses.
“ADD is a weird thing, because as I take this year to learn more about my brain and more about how my brain works and other people’s brain works, the thing I’ve learned the most is it’s less of a complete disorder and just a really big difference in the way the brain works,” she says.
Understanding that some people’s brains work differently than how society would like them to work can make a difference in how people view their own mental health issues.
“And it just doesn’t completely fit in with the way that society works. You have to figure out to do that,” she says.
Melissa Ray is intentionally open about their experience with mental illness.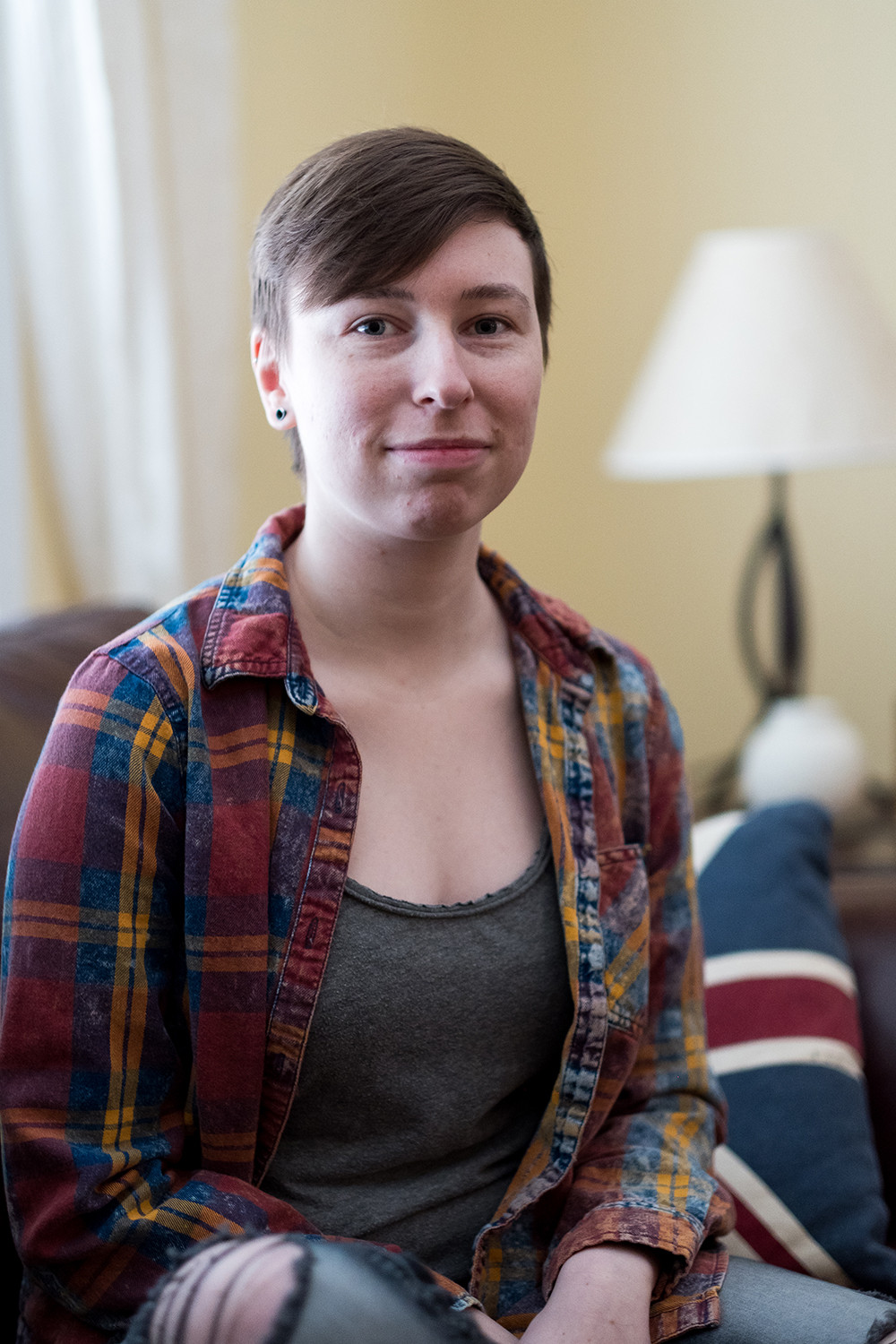
Heaman-Warne says there are a few different ways mental health can look, and it’s different for each person.
“I think it’s really complex for each person, and there is some mental illness that is organic in the brain,” he says. “And we need medication for the brain to have a healthy balance of chemicals.
“And I think there are other mental health challenges that we have that are much more personal and relational and experiential that counselling is really effective for. And there’s some that cross over between the two.”
Reaching out to a community, whether publicly or on social media, can be a good starting point when someone is starting to look for help.
Ray says when they started talking openly about their mental illness on social media, they started to see how many other people were also affected by the same thing.
“A lot of people reached out to me for support. A lot of people reached out to me about where to go to start medication, and that’s how I was able to start medication,” they say. “I’ve had people ask me for advice, especially with the medicinal marijuana and where to go, and counselling and stuff. It’s just been really nice to find community when you really open up about it.”
Published in Volume 72, Number 15 of The Uniter (January 25, 2018)