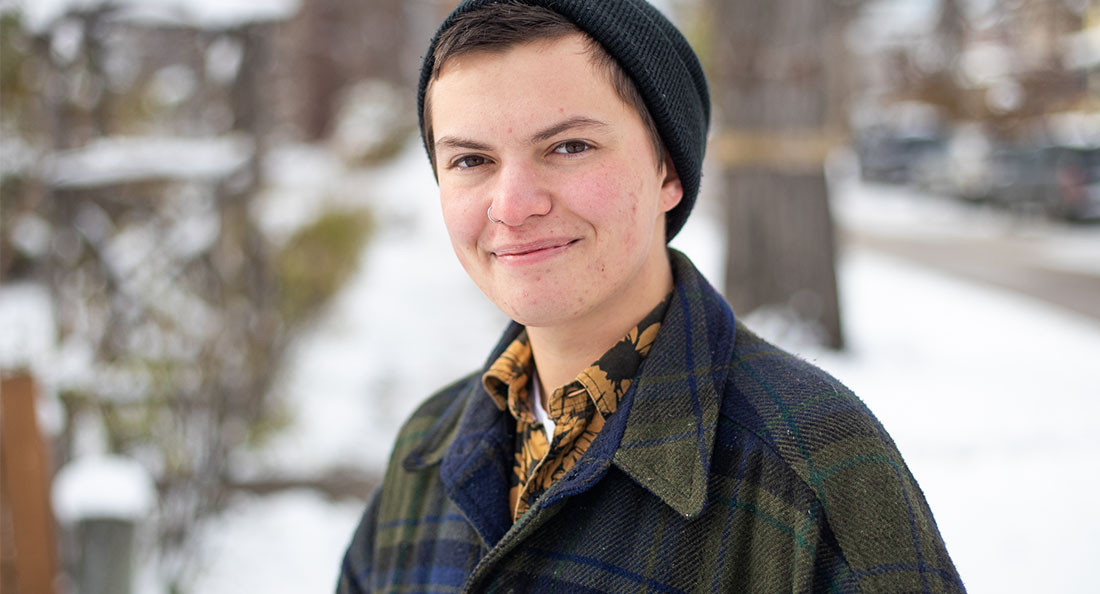Breaking down barriers to trans healthcare
Embracing informed consent can decrease wait times for gender-affirming care
EDITOR’S NOTE: We generally try to avoid interviewing our friends, family members or loved ones at The Uniter. However, given that Winnipeg’s transgender community is a small and close-knit one, this story would have been impossible to tell without our reporter speaking to close friends and community members. We felt the importance of the story necessitated an exception to the rule.
“On a scale from zero to 10, where zero is being a woman and 10 is being a man, how much do you feel like a man?”
This may sound like a question ripped from the pages of a teen magazine or an online quiz, but, until recently, it was one of the first questions encountered by many patients of the Trans Health Klinic, the only dedicated provider of transition-related healthcare in Manitoba for patients over the age of 14.
Ren Samuels’ intake appointment at Klinic was several years ago, but he still recalls the emotional experience of trying to answer this question.
“This was my first contact with anybody about this sort of care,” Samuels says. He waited a year between initially reaching out to Klinic and attending his first appointment.
“I remember being kind of nervous that if I didn’t have the right answer to this question, that I wouldn’t be able to access the care that I knew I wanted and did end up saving my life.”
Simon Pensato was asked the same question at his intake in the summer of 2020.

When Simon Pensato was asked to rate his gender identity on a scale of zero to 10, he “sort of took offense ... Women are not zeros!”
“I sort of took offense to that, you know, as a feminist,” he says, laughing. “Women are not zeros!”
Beyond being described as memorably bizarre by a number of interviewees, Pensato says questions like these can also be alienating for those who aren’t thinking about their gender in relation to manhood or womanhood.
“I was identifying very strongly as being nonbinary at the time but also trying to be recognized as a man at work,” he says. “It’s very difficult to feel like a 10 on that scale when you’re constantly being misgendered.”
Pensato’s and Samuels’ reactions provide anecdotal support to a trend documented in an AMA Journal of Ethics article by trans healthcare professionals Dr. Timothy Cavanaugh, Ruben Hopwood and Cei Lambert.
“Some patients might feel tempted to tell a stereotypical narrative of gender identity development and dysphoria in which their authentic gender is described in binary terms,” the trio argues, “even if this narrative would not truly represent their authentic gender identity.”
Samuels and Pensato both report being generally satisfied with the care they received at Klinic. Moreover, Klinic has put in significant work in recent months to ensure patients undergoing the intake process are given the space to articulate their gender identity on their own terms.
Klinic is on the path to significant improvements, but a legacy of frustrating experiences nonetheless remains. These experiences point to two interrelated issues which together present the biggest remaining barriers to high-quality trans healthcare in Manitoba: wait times and gatekeeping.

Cubes Endurance in her Winnipeg apartment
Wait times
Samuels was dealing with intense depression and gender dysphoria when he took the often-stressful initial step to contact Klinic about hormone replacement therapy (HRT), which amplified the difficulty of hearing he’d have to wait.
“You’ve made that decision. You’ve jumped through all the phone tag, and then hearing ‘Oh, yeah, we’ll probably get back to you in like a year.’ ... It sucked,” he says. “It feels very bleak.”
In August, CBC Manitoba’s Bryce Hoye reported wait times for gender-affirming care in Manitoba had reached one-and-a-half to two years, although Klinic’s 2022-23 Annual Report says internal reallocation of resources and an injection of $490,000 of provincial funding in May has allowed for expanded service hours to help address the backlog.
It took eight months for Cubes Endurance to get on feminizing hormones through Klinic. She says the complete lack of information from Klinic in between her initial call and first appointment was “nerve-racking.” She says an online portal with basic information would’ve helped reassure her that she hadn’t been forgotten.
I have likewise experienced Klinic’s inconsistent communication firsthand. My second follow-up for HRT, which is supposed to take place after three months, instead took 18. The wait only resolved itself when I contacted them after several faxes from my pharmacy went unanswered. To add insult to injury, they then refused to refill one of my prescriptions until the appointment, because it had been too long since the last follow-up.
Pensato also struggled to get information from Klinic while waiting unspecified amounts of time for appointments. In his case, an internal miscommunication resulted in a completed psychological assessment for top surgery not being sent in for several months, further delaying an already cumbersome process.
Gatekeeping
Trans people pursuing gender-affirming surgery in Manitoba need at least one, and sometimes two, psychological assessments from approved providers to confirm gender dysphoria. Once this diagnosis is on file, further surgeries still require a referral letter to ensure the patient understands what to expect.
However, Pensato says trans people often end up coming into these appointments knowing as much or more than their health providers. He recalls an appointment where a clinician incorrectly told him that masculinizing hormones would make him infertile.
Gender dysphoria is inherently personal and subjective. As argued by Cavanaugh et al., there are no biological markers or psychological screenings that can produce evidence more reliable than trans people’s self-reporting of our experience. Practices which value those screenings above our own understandings are the core of what many of us consider to be gatekeeping of trans healthcare.
University of Alberta assistant professor Florence Ashley argues that because of trans people’s “epistemic authority” over their mental experience of gender dysphoria, requirements for psychological assessment represent the pathologizing of normal human variance in a manner unsupported by evidence.
“Mental-health referral requirements fail to recognize the value of trans self-actualisation and, based on my experience with trans communities, will frequently be experience(d) as dehumanizing by those who do not fall under a pathologizing gender-dysphoria model,” Ashley writes.
Endurance says the persistence of gatekeeping practices are emblematic of a tendency for the healthcare system to be unwilling to recognize the enormous variety of circumstances patients experience. She suspects the bureaucracy trans people must navigate to access care serves partly as a “throttling mechanism” to mitigate strain on an under-resourced system.
“There (are) a lot of issues with the trans system that take the power away from the person and (put) it into the psychiatrist’s or the doctor’s hands,” she says. “We have an overworked system, and we’re using that as a gate to prevent trans care from occurring properly.”
After the first two to three years of treatment, Klinic will typically try to refer trans patients’ subsequent monitoring and dosage adjustments to their family doctors. Endurance fears there isn’t adequate knowledge about trans healthcare dispersed within the system to ensure overworked doctors are equipped to meet trans patients’ needs.
“You’re trusting that a doctor doesn’t fuck anything up for you,” she says. “I can tell you from personal experience, I have been screwed over by my doctor because he was too busy, and it resulted in almost two years of memory loss, mania, hypersexuality and debt. That’s all because the doctor couldn’t realize what was happening.”

“There (are) a lot of issues with the trans system that take the power away from the person and (put) it into the psychiatrist’s or the doctor’s hands.” - Cubes Endurance
Progress
Long wait times and excessive gatekeeping are endemic issues within trans healthcare, particularly in countries with public systems. Rather than needing to reinvent the wheel to innovate solutions, trans journalist and advocate Erin Reed says Manitoban decision-makers should look at other jurisdictions’ successes in expanding the informed-consent care model as a means of easing pressure on under-resourced systems and improving patient outcomes.
“Hormone therapy doesn’t require a huge evaluation to do. It’s not a big, huge deal,” she says. “I have to imagine that there’s at least one doctor in all of Manitoba that’s going to be like, ‘Trans people, I care about them. Maybe I can look this up and provide the basic care.’”
Reed says many jurisdictions in the United States have drastically reduced wait times by empowering various different kinds of healthcare providers who already administer hormones for cisgender patients, such as fertility clinics and centres for reproductive and sexual health, to also provide HRT.
Expanding on the connection between trans healthcare and reproductive health, Ashley says the provision of abortions is another clear example of how informed consent is the only ethical way to administer certain kinds of care.
“For somebody who’s seeking an abortion, if (a doctor) were to try to assess if they’re really dysphoric about the potential of having a pregnancy ... (a doctor is) not in any position to assess that,” they say. “There’s really nothing to assess. It’s more about people living out their lives and being able to do so.”
Haran Vijayanathan, Klinic’s community health and wellness director, moved to Manitoba three months ago. Having spent 20 years working with the LGBTQ+ community in Ontario, he was taken aback by how many more hurdles an individual faces seeking gender-affirming care in Manitoba relative to the Ontario system, which makes use of small informed-consent clinics.
He says the change in government is a great opportunity for Klinic to not only secure more funding, but also to instigate the kinds of structural change Reed and Ashley advocate for.
“There’s a lot of barriers in place, and they’re all systems barriers,” he says. “It would be great to sort of sit down and have a conversation about the systems that are in place currently and understand what that looks like from the medical end ... from the policy end, on their end and how do we bring down some of those barriers?”
Ashley Gawne is one of the trans health program’s peer support workers. She is “hopeful” that the expansion of her position, alongside the hiring of two more trans people into positions in peer support and social work, will help strengthen Klinic’s relationship with the trans community.
“There have been barriers in the past where individuals seeking care through here get a lot of cis allies,” she says. “It’s nice to see trans representation, especially within a trans health clinic, because … the nuance of being trans speaks volumes, right?”
Gawne is alluding to the fact that a core aspect of how trans people find community with one another is through transition-related knowledge sharing, and many of the most robust sources of information about trans healthcare come from within the community.
Without my trans friends and loved ones, I wouldn’t have known to ask for a higher dose of estrogen, nor realized that suddenly starting to cry all the time meant that the HRT was working. Without a role model like Reed, I wouldn’t have had the inspiration to use this platform to tell stories about our community. We are experts in our own experiences, and we take care of us.
It’s too early to say what structural impacts Klinic’s recent changes will make to the landscape of trans healthcare in Manitoba, but Endurance says one recent experience with Klinic suggests they may be getting closer to providing the supports she’d most like to see.
“It was one clinical provider that was trans, and they are absolutely phenomenal,” she says. “I think her name is Ashley.”
Published in Volume 78, Number 08 of The Uniter (November 2, 2023)